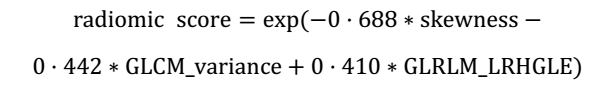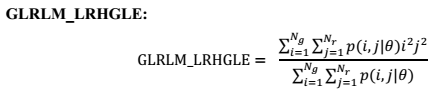An individualized imaging biomarker for treatment decision in locoregionally advanced nasopharyngeal cancer: a substudy of the randomized controlled trial
We aimed to use pretreatment MR imaging and clinical characteristics of locoregionally advanced Nasopharyngeal carcinoma (NPC) from a retrospective cohort to develop an individualized radiomic biomarker for screening of those who benefit most from additional Induction chemotherapy (ICT). Then, we use data from randomized controlled trial to validate the performance of the biomarker and try to recommend clinical decision support system (CDSS) for the best choice between concurrent chemoradiotherapy (CCRT) and ICT + CCRT in locoregionally advanced NPC.
The selected radiomic features were used to train a multivariable Cox proportional hazards model with failure-free survival as the endpoint using the modified covariate method. Radiomic scores from the model were calculated by taking the difference of treatment outcome to additional ICT and then converted to binary scores, which we have termed the Induction Chemotherapy Outcome Score (ICTOS), using a cutoff of 0.
Our CDSS, which combined radiomic ICTOS with clinical prognostic factor together, can classified advanced locoregional NPC into three group and recommended according individual therapies: (1) High ICTOS: ICT +CCRT, (2) Low ICTOS and low risk: CCRT alone. (3) Low ICTOS and high risk: clinical trials. This is the first time that clinical prognostic factors and predictive factors have been integrated to guide the individualized treatment of nasopharyngeal carcinoma.

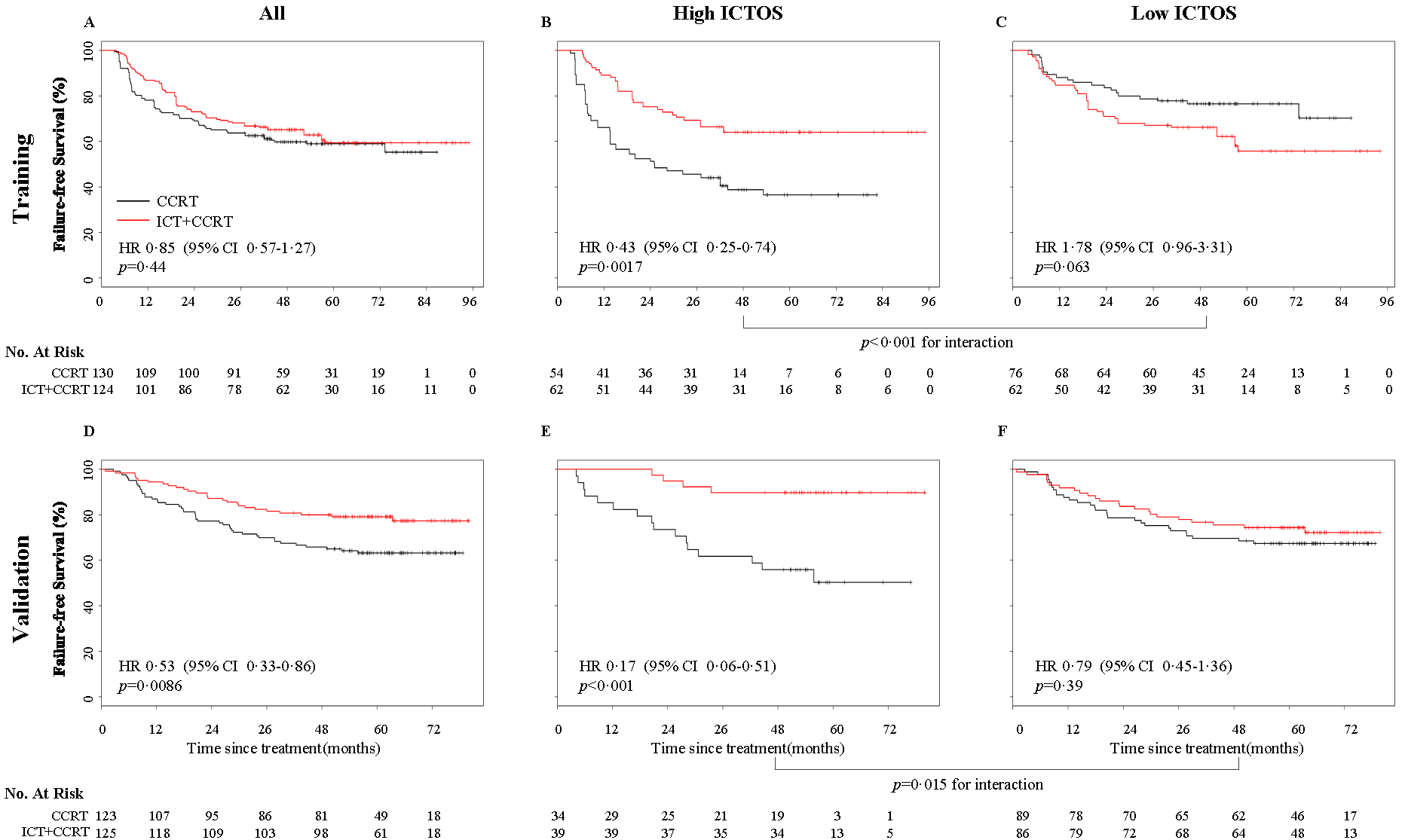
Figure 1. Failure-free survival in the training and validation cohorts stratified by low and high ICTOS

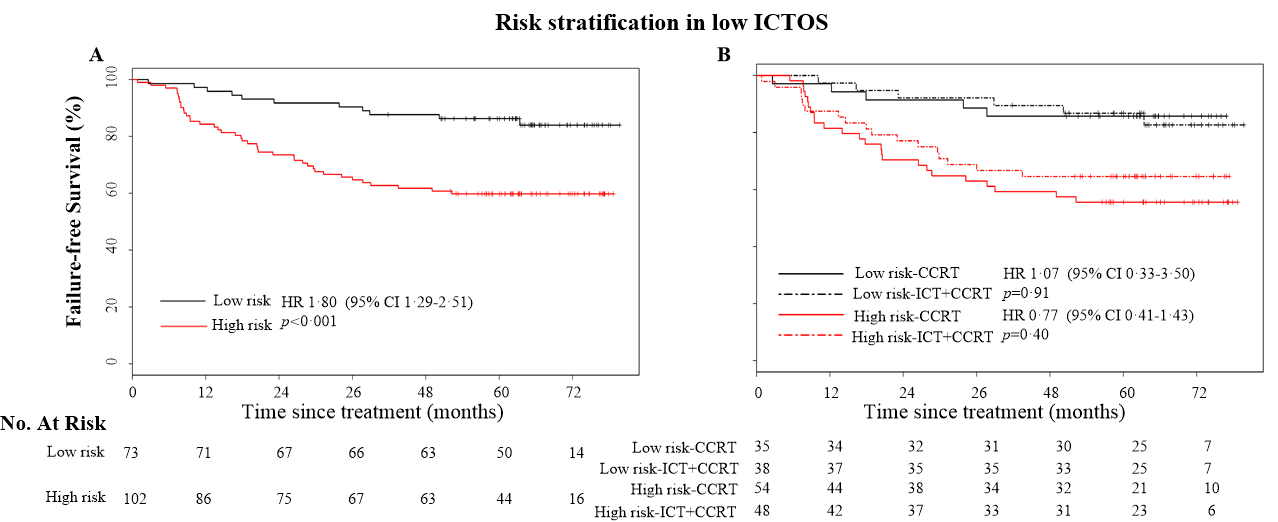
Figure 2. Stratification analysis of patients with low ICTOS in the prospective validation cohort.
Radiomic score calculation formula
After features selection, skewness, variance from GLCM (GLCM_variance) and Long Run High Gray Level Emphasis from GLRLM (GLRLM_LRHGLE) were identified by a multivariable cox proportional hazards model using the modified covariate method. Radiomic score from the model could be obtained: